Postpartum Digestive Issues: Why Symptoms Don’t Go Away and What to Do

If your digestion hasn’t felt the same since having a baby, you’re not imagining it.
We regularly work with women months (or even years) postpartum who expected things to go back to normal, but are still dealing with:
- Bloating that doesn’t match what they eat
- Constipation or irregular bowel movements
- Acid reflux or nausea
- A gut that feels more sensitive or unpredictable
In the early weeks after birth, some digestive changes are expected.
But if your symptoms haven’t gone away, or they keep coming back, there’s a reason.
In this blog post we’ll cover:
- The four main reasons postpartum digestive issues happen
- Which symptoms are normal, which aren’t, and a typical postpartum timeline
- The two tests we recommend
- How we support postpartum digestion naturally
What Most Women Are Told
Most women are told their symptoms are due to hormones, stress, or just part of recovery.
So they try adding more fiber, taking probiotics or magnesium, or cutting out certain foods.
Sometimes that helps.
Often it doesn’t.
Because these approaches
don’t address what’s actually driving your symptoms.

What We See in Our Practice
After working with 700+ women, we’ve found that postpartum gut issues are almost always multifactorial.
That means multiple root causes are happening at the same time.
While many factors can be involved, these are the four most common drivers we see.
1. Hormone Shifts
During pregnancy, high progesterone slows digestion (this is why constipation and reflux are common).
After delivery,
estrogen and progesterone drop abruptly, and that sudden shift can disrupt gut rhythm, stool consistency, and sensitivity.
Breastfeeding, sleep loss, and stress create even more disruption via the gut–brain connection.
This can make digestion more reactive or unpredictable, even if your diet hasn’t changed much.
2. Microbiome Disruption (A Big One)
Pregnancy, labor, antibiotics, and stress all shift the gut microbiome.
We often see postpartum women with:
- Reduced “good” commensal gut bacteria
- Overgrowth of gas-producing and/or inflammatory gut bacteria
- Increased gut inflammation
- Low levels of digestive enzymes
These imbalances can drive bloating, acid reflux, heartburn, upset stomach, constipation, or loose stools, especially if you had gut issues before pregnancy.
3. Pelvic Floor Changes (Even If You Had a “Normal” Delivery)
Your pelvic floor plays a huge role in bowel function, not just bladder control.
After pregnancy and delivery, these muscles may be weak, tight, or poorly coordinated. Nerves involved in bowel function can also be affected.
This can lead to constipation, incomplete emptying, urgency, or a feeling of being “blocked,” even if your delivery was uncomplicated.
4. C-Section and Pain Med Side Effects
If you had a C-section, anesthesia can slow gut movement, pain medications can worsen constipation, and surgery changes abdominal pressure and coordination.
These effects are common early on, but in some cases they continue longer than expected without targeted support.

What’s Normal Postpartum (and What’s Not)
In the first 2-6 weeks postpartum, it’s common to experience changes in digestion.
This can include:
- Delayed bowel movements
- Constipation or straining
- Gas and bloating
- Loose stools or urgency
- Mild hemorrhoids
- Discomfort with bowel movements
These symptoms should gradually improve as your body heals, and typically shouldn't last for more than six weeks.
If you're still experiencing symptoms months after giving birth, it’s a sign to look deeper.
We commonly see these patterns in women who benefit from functional medicine support:
- Constipation that persists for months
- Bloating that feels disproportionate to what you’re eating
- Stomach discomfort that fluctuates without a clear trigger
- Alternating constipation and loose stools
- Feeling like your digestion never returned to pre-pregnancy baseline
- Symptoms that improve temporarily, then come back again
At that point, your body isn’t just recovering. It’s stuck.
What to Do If Your Symptoms Aren’t Improving
Because postpartum gut issues are often multifactorial, guessing rarely works.
One of the biggest frustrations we hear from postpartum women is that they feel like they’ve already tried everything — more fiber, probiotics, magnesium, or cutting out certain foods.
Sometimes this helps, but the improvements don’t last.
Because without understanding what’s driving your symptoms, it becomes trial and error.
Rather than guessing, we use
comprehensive bloodwork and a
GI MAP stool test to understand what’s driving your symptoms.
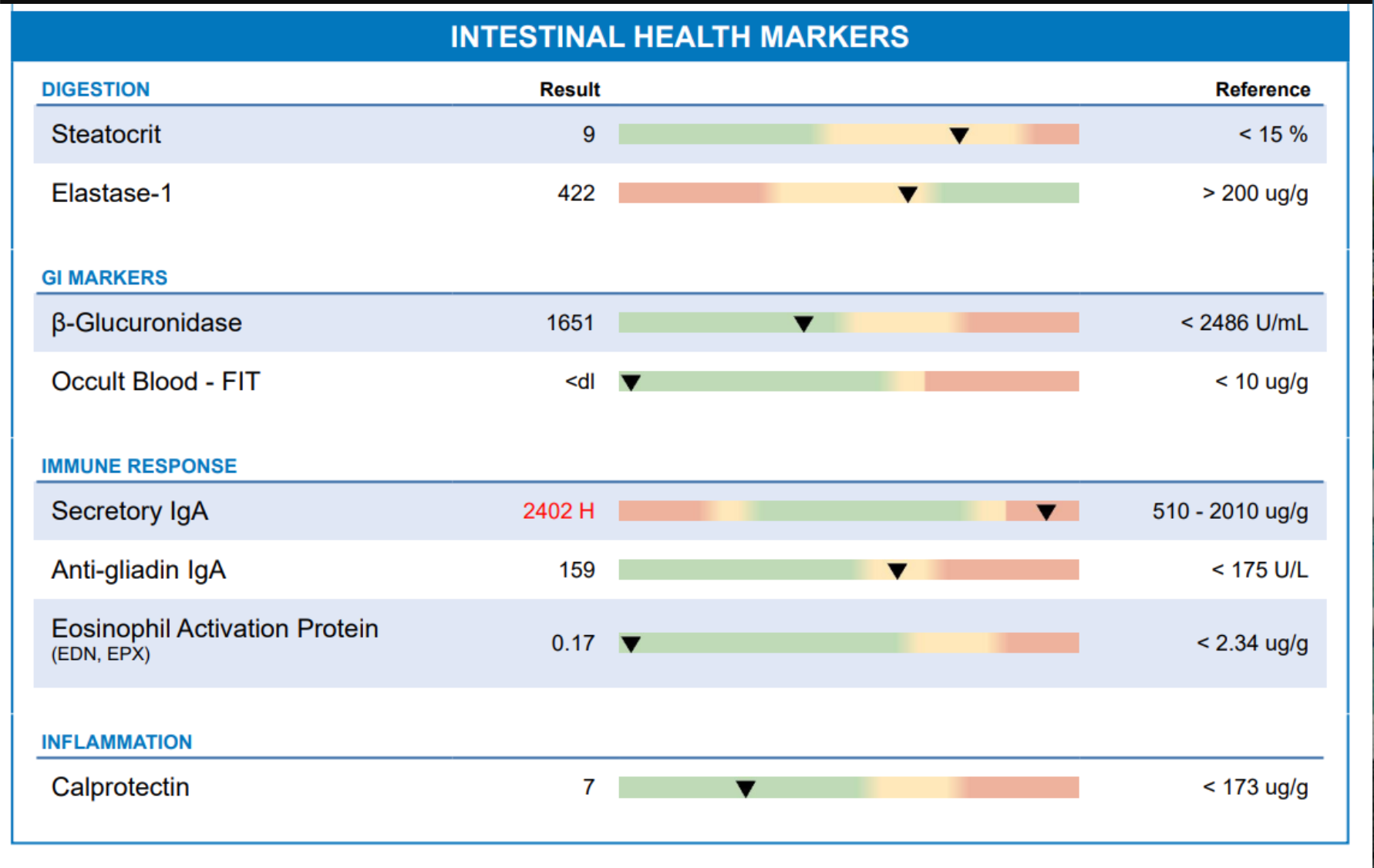
These tests help us assess:
- Gut inflammation
- Bacterial or fungal overgrowth
- Digestive enzyme production
- Thyroid function
- Nutrient status
- Gut–hormone interactions
This allows us to be targeted and efficient, so you’re not eliminating foods you don’t need to eliminate or taking supplements you don’t need.
Postpartum gut issues are rarely “just part of motherhood.”
There’s almost always a root cause.
And once you know what that is, the path to healing becomes much clearer.
How We Support Postpartum Digestion (and Why It Works)
1. Targeted Nutrition
Rather than following a restrictive diet, we tailor nutrition based on your specific gut pattern.
This often includes gradually increasing fiber, supporting hydration with electrolytes, and incorporating specific nutrients or probiotic foods based on your needs.
The goal isn’t to eliminate more foods, but to support digestion in a way your body can actually tolerate.
2. Hormone and Metabolic Support
After pregnancy your body is recalibrating multiple systems at once, including hormones, thyroid function, blood sugar, and nutrient levels.
All of these directly affect digestion.
Low thyroid can slow motility. Blood sugar swings can worsen nausea, reflux, and urgent trips to the bathroom. Nutrient deficiencies can impact enzyme production and gut function.
This is why we don’t look at the gut in isolation.
3. Nervous System Support
Your gut listens to your nervous system.
Sleep deprivation, stress, and mood changes can all make digestion more sensitive or unpredictable.
Supporting the nervous system may include improving sleep quality, supporting stress resilience, and incorporating simple strategies that help regulate the gut–brain connection.
4. Pelvic Floor Support
Pelvic floor physical therapy isn’t just for bladder leaks or pain with sex.
It can also help with constipation, incomplete emptying, gas trapping, urgency and leakage by improving muscle coordination and nerve signaling.
When appropriate, we refer clients to a trusted pelvic floor physical therapist and see meaningful improvements when this is addressed alongside gut health.

Final Thoughts
Postpartum digestive issues are common, but that doesn’t mean you have to live with them.
If you’re months (or even years) postpartum and still dealing with symptoms, it’s not a failure. It’s a signal.
And with the right support, your body can move forward.
Want to Get to the Root Cause?
If you’re still dealing with digestive issues months postpartum, it may be time to look deeper.
We help clients identify what’s driving their symptoms through advanced testing and personalized care, so they’re not guessing.
🔍 Learn more about our Wellness Blueprint
📞 Book a 20-minute discovery call to find out if it’s a good fit
📍 Plate & Canvas is based in Austin, TX, and 100% virtual — supporting holistic health nationwide.
Continue Reading